HIPAA Compliant Telehealth During Public Health Emergencies – Expert Solutions From Secure Waste
Secure Waste explains that healthcare providers can deliver HIPAA-compliant telehealth services during public health emergencies. Understand enforcement discretion, privacy considerations, and compliance best practices.
Welcome to Secure Waste, the premier biohazard disposal management company serving the DC-MD-VA region, commonly referred to as the DMV.
With over 30 years of experience, Secure Waste has dedicated itself to assisting healthcare organizations across Washington, D.C., Maryland, and Virginia with safe, compliant biohazard waste management, sharps disposal, and pharmaceutical waste services.
In light of recent public health emergencies, particularly the COVID-19 pandemic, it’s crucial to discuss the evolving landscape of healthcare and the impact of telehealth.
The introduction of telehealth has revolutionized how medical services are delivered, making healthcare more accessible and safer for everyone. It allows patients to receive medical advice, consultations, and follow-up care from the comfort of their homes, significantly reducing the risk of exposure to infectious diseases.
At Secure Waste, we prioritize community and environmental safety and remain committed to providing comprehensive solutions tailored to healthcare providers’ unique needs. We want to invite you to learn more about our services and how we can support your organization in these challenging times.

The COVID 19 pandemic has highlighted the importance of public health emergencies and the global response to infectious diseases This unprecedented situation has prompted nations and organizations to collaborate to monitor manage and mitigate the viruss impact on communities worldwide Understanding the implications of such emergencies is crucial for enhancing public health preparedness and ensuring the safety and well being of populations during future health crises
HIPAA Compliant Telehealth During Public Health Emergencies
How Healthcare Communication Changed During the Pandemic
Public health emergencies have a way of reshaping healthcare delivery almost overnight.
During the COVID-19 pandemic, healthcare organizations were forced to rethink how they interacted with patients while maintaining safety, access, and continuity of care. In-person visits were limited, elective procedures were postponed, and providers needed alternative ways to deliver medical guidance and treatment.
Telehealth emerged as a critical solution. Remote communication allowed providers to continue caring for patients, share public health information, and reduce unnecessary exposure risks. At the same time, healthcare organizations faced uncertainty about how privacy regulations applied in a rapidly evolving environment.
To address these challenges, federal authorities introduced temporary flexibility to support care delivery while maintaining core privacy protections.
Understanding Telehealth in a Healthcare Setting
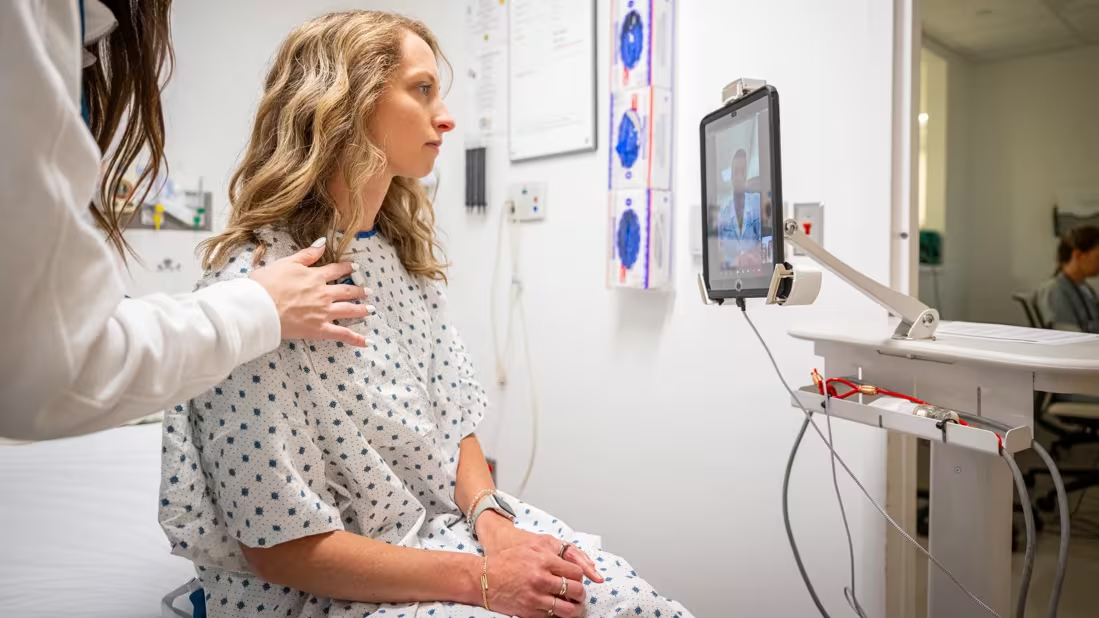
Telehealth refers to the use of electronic and telecommunication technologies to support long-distance clinical care, patient education, public health activities, and healthcare administration. These services may include audio calls, video consultations, secure messaging, and remote monitoring tools.
Telehealth interactions should take place in private settings whenever possible. For example, a healthcare provider may conduct a consultation from an office or clinic while a patient participates from their home or another healthcare location. Maintaining privacy remains a foundational expectation, even when care is delivered remotely.
Telehealth does not entirely replace traditional care models, but it provides flexibility during emergencies and expands access for patients who cannot attend in-person appointments safely.
Temporary HIPAA Enforcement Discretion Explained
During the COVID-19 public health emergency, the Office for Civil Rights announced it would exercise enforcement discretion related to certain provisions of the HIPAA Privacy Rule.
This decision allowed healthcare providers to offer telehealth services in good faith without facing penalties for specific noncompliance issues related to remote communication.
This discretion applied to all covered healthcare providers who used telecommunication technologies to deliver telemedicine services during the declared emergency. Importantly, it applied regardless of whether the care being provided was directly related to COVID-19.
The goal was to remove barriers that could prevent patients from receiving timely care while still encouraging responsible handling of protected health information.
Who Does the Enforcement Discretion Cover
Enforcement discretion was applied broadly across healthcare settings. Physicians, dentists, mental health professionals, clinics, and hospitals were all permitted to use telehealth platforms to serve patients during the emergency period.
The discretion remained in effect until the Department of Health and Human Services declared the public health emergency had ended. Providers were still expected to act in good faith and take reasonable precautions to protect patient privacy whenever possible.
This flexibility helped ensure continuity of care at a time when traditional healthcare delivery was severely disrupted.
Telecommunication Technologies and Privacy Considerations
Healthcare providers were permitted to use a range of telecommunication tools to communicate with patients, provided the technologies were not public-facing. Acceptable options included phone calls, text messaging, and video conferencing platforms that offered private communication channels.
Public-facing platforms designed for broadcasting were discouraged. The focus remained on tools that enabled one-to-one or controlled-group communication.
Providers were encouraged to inform patients if third-party applications were being used and to explain any potential privacy risks associated with those platforms. Transparency helped patients make informed decisions about their care.
If protected health information was intercepted or compromised during transmission, regulators indicated they would consider all relevant facts when evaluating whether the provider acted in good faith.
Sharing Protected Health Information During a Public Health Emergency
Another key component of the enforcement discretion involved the sharing of protected health information related to COVID-19. Public health agencies and oversight organizations required timely access to accurate data to manage resources, track outbreaks, and coordinate response efforts.
Healthcare organizations were permitted to share relevant information with public health departments, emergency operations centers, and regulatory authorities. This sharing supported public health planning and potentially saved lives.
In addition, business associates were allowed to share necessary information without fear of HIPAA violations during the emergency period. This flexibility improved communication between healthcare providers, partners, and government agencies.
Changes Affecting Substance Use Disorder Records
During the public health emergency, certain restrictions related to substance use disorder records were temporarily relaxed when a medical emergency existed. Providers were allowed to share patient-identifying information when necessary to address an immediate health risk.
Separately, legislative changes expanded long-term alignment between substance use disorder privacy rules and existing HIPAA Privacy and Security standards. These updates were designed to improve care coordination while maintaining appropriate protections for sensitive information.
Healthcare organizations were advised to monitor guidance closely and prepare for future implementation requirements as regulations evolved.
Maintaining Compliance Beyond Emergency Flexibility
While enforcement discretion provided temporary relief, healthcare organizations were still responsible for maintaining strong compliance practices. Acting in good faith included using reasonable safeguards, educating staff, and documenting telehealth policies and procedures.
Organizations that relied heavily on telehealth during emergencies benefited from reviewing their privacy programs and identifying opportunities for improvement. Clear policies, staff training, and technology assessments supported long-term compliance and patient trust.
As emergency declarations expire, healthcare providers must ensure their telehealth practices fully comply with HIPAA requirements.
The Role of Compliance Partners in Healthcare Operations
Managing compliance during periods of rapid change is challenging. Regulations evolve, guidance updates are issued, and operational demands increase. Healthcare organizations benefit from working with experienced partners who understand regulatory environments and operational risk.
While telehealth compliance focuses on privacy and security, healthcare operations also involve other regulated areas such as medical waste handling, documentation, and environmental responsibility.
Healthcare providers across the United States work with Secure Waste to support compliant and responsible waste management practices. Reliable partners help organizations stay aligned with regulatory expectations while focusing on patient care.
Building Resilient Healthcare Systems
Public health emergencies highlight the importance of flexibility, preparedness, and accountability. Telehealth has become an essential tool for maintaining access to care, and compliance remains a critical foundation for trust and safety.
Healthcare organizations that invest in strong compliance programs and professional partnerships are better equipped to navigate future disruptions. Clear policies, informed staff, and reliable vendors create resilience across clinical and operational functions.
By balancing innovation with responsibility, healthcare providers can continue delivering care while protecting patient information and meeting regulatory obligations.

Expert Medical Waste Management: With over 25 years of industry experience, Secure Waste is a trusted local leader in hazardous and biohazardous waste disposal across Maryland, Virginia, and Washington, D.C. Specializing in medical waste management, sharps needle disposal, and biohazard waste removal, the company ensures full compliance with federal, state, and local regulations while prioritizing environmental sustainability.
The company also offers additional services, including secure document shredding and sharps container sales, providing comprehensive solutions for healthcare facilities and businesses. Our cost-effective services help clients maintain regulatory compliance without unexpected costs.
With a commitment to customer satisfaction, Secure Waste offers tailored waste management plans that align with industry best practices. Their team of experts provides reliable, timely, and compliant services, making them the preferred choice for medical waste disposal. For a free waste quote or more information, visit www.securewaste.net